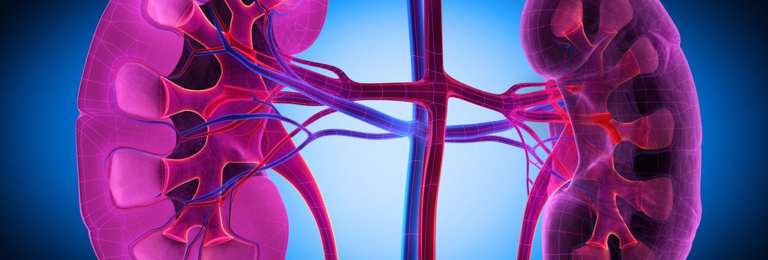
Chronic renal failure
Kidney failure means that your kidneys are not working properly. Chronic renal failure (CRF) means that kidney function slowly worsens over time. High blood pressure and diabetes are two common causes of CRF. There is no cure for CKD, but steps can be taken to preserve function for as long as possible. Advanced kidney failure requires dialysis or a kidney transplant.
What is kidney failure ?
Having kidney failure means that the kidneys are damaged and are not working the way they should. Kidney failure is called "chronic" because kidney function slowly worsens over time. Kidney disease leads to kidney failure, which is also called end-stage renal disease. At this point, you will need dialysis (artificial filtration) or a kidney transplant.
What do your kidneys do?
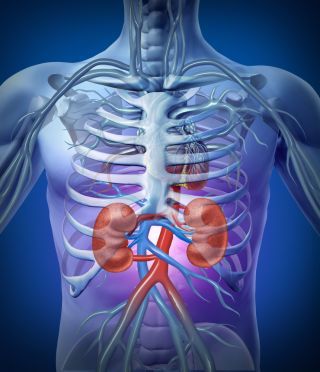
You have two kidneys. They are bean-shaped organs found in the back of the abdomen, on either side of the spine, just below the ribcage. Each kidney is about the size of your fist. Your kidneys have many jobs, but their main job is to filter (clean) your blood, removing toxins (waste) and excess salt and water in the form of urine. If your kidneys are damaged and don't work the way they should, waste can build up in your blood and make you sick. Your kidneys also balance the amount of salts and minerals in your body, make hormones that control your blood pressure, make red blood cells, and keep your bones strong.
Are there stages of chronic renal failure?
Yes, there are five stages of kidney disease. The phases are based on how well your kidneys can do their job: filtering waste and extra fluid from your blood. Stages range from very mild (stage 1) to end-stage renal disease (stage 5). Health professionals determine the stage of kidney function based on the glomerular filtration rate (GFR). Your GFR is a number based on the amount of creatinine, a waste product, in your blood, along with other factors, such as age, race, and gender.
The stages of any kidney disease include:
- Stage I. Your GFR is above 90 but below 100. At this stage, your kidneys have little damage and are still functioning normally.
- Stage II. His GFR is between 60 and 89. His kidneys are more damaged than in stage I, but they are still working well.
- Stage III. Your GFR is between 30 and 59. You may have mild or severe loss of kidney function.
- Stage IV. Your GFR is between 15 and 29. You have severe loss of kidney function.
- Stage V. Your GFR is below 15. Your kidneys are in kidney failure or close to kidney failure.
Who is at risk of developing chronic kidney disease?
About 37 million people in the United States are living with chronic kidney disease. Anyone can have chronic kidney disease. You are more at risk of chronic kidney disease if you:
- He has diabetes.
- You have high blood pressure.
- He has heart disease.
- You have a family history of kidney disease.
- You have an abnormal kidney structure.
- You are over 60 years old.
- He has a long history of taking pain relievers, including over-the-counter products like aspirin and ibuprofen.
SYMPTOMS AND CAUSES
Kidney disease occurs when the kidneys are damaged and cannot filter the blood. Damage can occur quickly, when caused by injury or toxins, or, more commonly, over the course of months or years.
High blood pressure (hypertension) and diabetes are the two most common causes of chronic kidney disease. Other causes and conditions that affect kidney function and can lead to chronic kidney disease include:
- Glomerulonephritis. This type of kidney disease involves damage to the glomeruli, which are the filtering units within the kidneys.
- Polycystic kidney disease. This is a genetic disorder that causes many fluid-filled cysts to grow in the kidneys, reducing the ability of the kidneys to function.
- hypertensive nephrosclerosis. Kidney damage caused by chronic hypertension.
- membranous nephropathy. This is a disorder in which your body's immune system attacks the debris filter membranes in your kidney.
- Blockages in the urinary tract due to kidney stones, enlarged prostate, or cancer.
- Vesicourethral reflux. This is a condition in which urine flows up ( refluxes) back up the ureters to the kidneys.
- Recurrent kidney infection (pyelonephritis).
- Diabetes-related nephropathy. This is the damage or dysfunction of one or more nerves, caused by diabetes, which usually causes numbness, tingling, muscle weakness, and pain in the affected area.
- Lupus and other immune system diseases that cause kidney problems, such as polyarteritis nodosa, sarcoidosis, Goodpasture syndrome, and Henoch-Schonlein purpura.
What are the symptoms of chronic kidney disease?
In the early stages of kidney disease, there are usually no obvious symptoms. As the disease worsens, symptoms may include:
- Need to urinate more frequently
- Tiredness, weakness, low energy level
- loss of appetite
- Swelling of hands, feet and ankles
- Difficulty breathing
- Blood in the urine; foamy urine.
- Swollen eyes
- dry itchy skin
- Difficult to focus
- Difficulty to sleep
- Numbness
- Nausea or vomiting
- Muscle cramps
- Hypertension
- skin darkening
What are the complications of chronic kidney disease?
If your kidneys aren't working properly, the rest of your body won't either. Some of the complications of chronic kidney disease include:
- Low number of red blood cells (anemia)
- Weak and brittle bones
- Drop
- Metabolic acidosis. This is a chemical (acid-base) imbalance in the blood caused by impaired kidney function.
- Hypertension
- Heart disease, including an increased risk of stroke and heart attack.
- High potassium (hyperkalemia), which affects the heart's ability to function properly
- High phosphorus (hyperphosphatemia)
- Fluid buildup, which causes swelling of the feet, ankles, and hands; fluid in the lungs
- erectile dysfunction, fertility problems
- Decreased immune response, increased risk of infection
DIAGNOSIS AND TESTS
How is kidney disease diagnosed?
Your doctor will read your medical history, perform a physical exam, ask about any medications you're currently taking, any symptoms you've noticed, and whether anyone in your family has kidney disease.
Your doctor will order blood tests, a urinalysis, and will also check your blood pressure.
Blood tests will check:
- Your glomerulofiltration rate (GFR). This describes how efficiently your kidneys filter your blood: how many milliliters per minute your kidneys filter. Your GFR is used to determine the stage of your kidney disease.
- Your serum creatinine level, which indicates how well your kidneys are removing this waste product. Creatinine is a waste product of muscle metabolism and is normally excreted in the urine. A high level of creatinine in the blood means that the kidneys are not working well enough to remove it in the urine.
- A protein urine test will look for the presence of protein (albumin) and blood in the urine. Well-functioning kidneys should not have blood or protein in the urine. If it does, it means your kidneys are damaged.
Other tests may include imaging studies to detect problems with the size and structure of the kidneys, such as ultrasound, magnetic resonance imaging (MRI), and/or computed tomography (CT). Your doctor may also order a kidney biopsy to detect a specific type of kidney disease or to determine the amount of kidney damage. In this procedure, which is performed under local anesthesia, a piece of kidney tissue is removed and examined.
MANAGEMENT AND TREATMENT
There is no cure for chronic kidney disease (CKD), but steps can be taken in early CKD to preserve a higher level of kidney function for a longer period of time. If you have reduced kidney function:
- Make regular visits to your doctor/nephrologist
- Check your blood sugar if you have diabetes
- Avoid taking pain relievers and other medicines that could make your kidney disease worse.
- Check your blood pressure levels
- Consult a nutritionist about helpful dietary changes. Diet changes may include limiting protein, eating foods that lower blood cholesterol levels, and limiting sodium (salt) and potassium intake.
- No Smoking
- Treat anemia (if present)
- Exercising/being active most days of the week
- keep a healthy weight
What medications are prescribed for people with chronic kidney disease?
Depending on the cause of your kidney disease, you may be prescribed one or more medications. Medications that your nephrologist may prescribe include:
- An angiotensin-converting enzyme (ACE) inhibitor or angiotensin receptor blocker (ARB) to lower blood pressure
- A diuretic to help your body get rid of excess fluid.
- Medications to lower cholesterol levels
- Erythropoietin, to make red blood cells if you have anemia
- Vitamin D and calcitrol to prevent bone loss
- Phosphate binder if your kidneys cannot remove phosphate
What is kidney dialysis?
Because there is no cure for chronic kidney disease, if you are in the late stages of the disease, you and your health care team should consider additional options. Advanced kidney failure, if left untreated, will lead to death. Options for end-stage chronic kidney disease include dialysis and kidney transplantation.
Dialysis is a procedure that uses machines to remove waste products from the body when the kidneys can no longer do this job . There are two main types of dialysis.
Hemodialysis: In hemodialysis, blood circulates through a machine that removes waste products, excess water, and salt. Then the blood returns to his body. Hemodialysis lasts three to four hours, three times a week, and is done in a clinic, hospital, or dialysis center.
Peritoneal dialysis: In peritoneal dialysis, a dialysis solution is put directly into the abdomen. The solution absorbs the debris and is then removed through a catheter. Fresh solution is added to continue the cleaning process. You can do this type of dialysis yourself. There are two types of peritoneal dialysis: continuous ambulatory peritoneal dialysis (CAPD), which involves changing the dialysis solution four times a day; and continuous cycle peritoneal dialysis (CCPD) which uses a machine to remove waste and automatically replenish fluid overnight.
What is the Kidney Transplant?
A kidney transplant involves inserting a healthy kidney into your body capable of performing all the functions that a defective kidney cannot. Kidneys for transplant come from two sources: living donors and deceased donors. Living donors are usually close relatives or sometimes spouses. This is possible because a person can live well with a healthy kidney.
Deceased donor kidneys usually come from people who donated their kidneys before they died by signing organ donor papers. All donors are carefully screened to ensure a proper match and to prevent communicable diseases or other complications.
PREVENTION
Is it possible to prevent kidney disease? Seeing your doctor regularly throughout your life is a good start in preventing kidney disease. About one in three people is at risk of kidney disease. Therefore, it is necessary to identify and control any risk factors for the development of kidney disease.
- Control your blood pressure. Normal blood pressure is 120/80
- Check your blood sugar if you have diabetes
- Follow a healthy diet. Follow a diet low in fat and salt
- No Smoking
- Be active for 30 minutes at least five days a week.
- keep a healthy weight
- Take over-the-counter pain relievers only as directed. Taking more than directed can harm your kidneys
OUTLOOK / FORECAST
If you have kidney disease, you can still live a productive life at home and at work and enjoy time with family and friends. To get the best possible outcome, it is important that you become an active member of your treatment team. Early diagnosis and appropriate treatment are important to slow the disease process, with the aim of preventing or delaying kidney failure.